Barrières en facilitatoren voor mHealth-programma diabetes en hypertensie in Ghana
Het Akoma Pa-programma is een mHealth-geïntegreerd zorgprogramma voor diabetes en hypertensie in Ghana. Via diepte-interviews met 30 implementatiemanagers en zorgverleners werden barrières en facilitatoren voor opschaling geïdentificeerd.
Abstract (original)
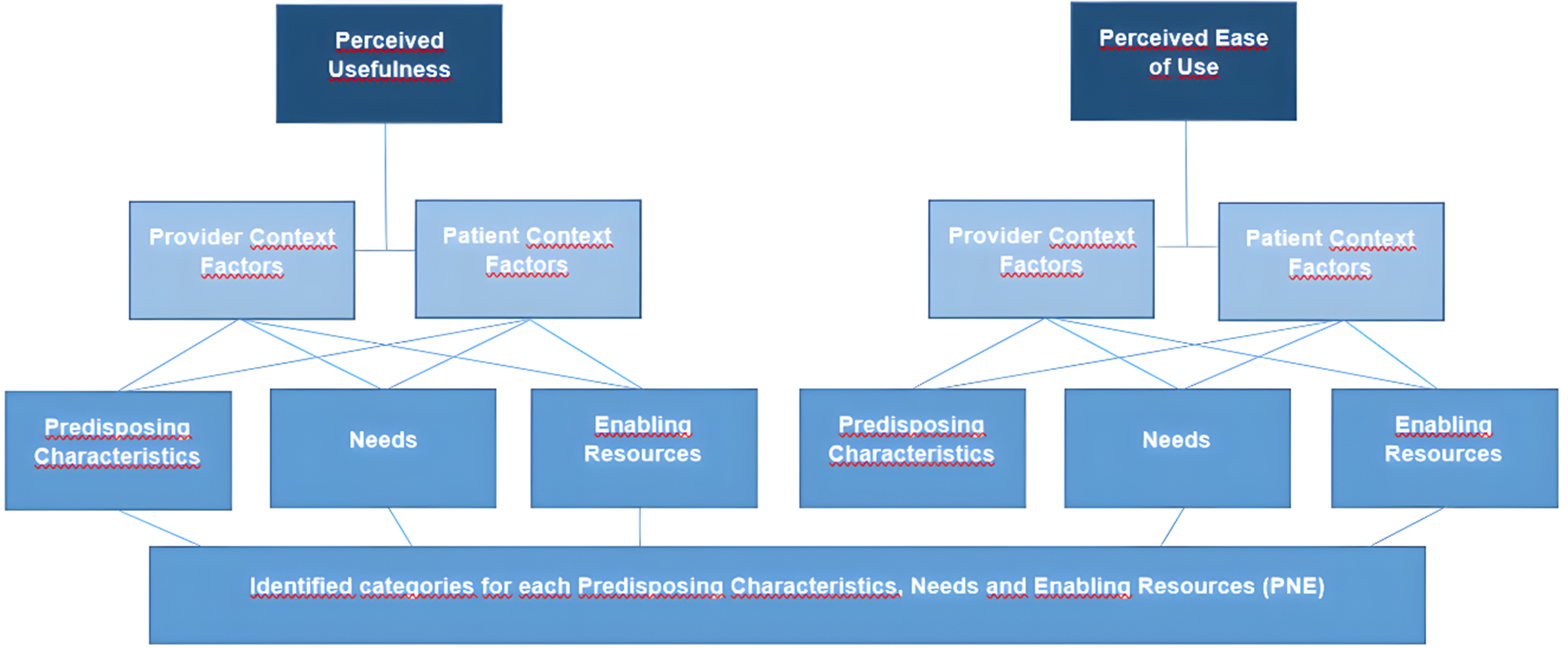
OBJECTIVE: To determine the barriers and facilitators to the implementation and scale-up of the Akoma Pa mHealth-based integrated care program for diabetes and hypertension in Ghana. METHODS: 30 implementation managers and healthcare providers (Akoma Pa champions) were interviewed in-depth based on their experience and ability to provide information on implementing and scaling-up the Akoma Pa program in February 2024. Participants were selected from the Christian Health Association Ghana healthcare facilities across Ghana. Thematic qualitative content analysis based on Kuckartz was used to identify recurring themes and categories, guided by the mHealth Predisposing Characteristics, Needs, and Enabling Resources (PNE) Framework. RESULTS: Participants identified 47 factors influencing the implementation and scale-up of the intervention, categorized into provider- and patient-level contextual factors. Findings were organized according to perceived usefulness and perceived ease of use, reflecting assessments of value, feasibility, and scale-up potential. Key enablers included mobile phone accessibility, provider engagement, and integration with the National Health Insurance Scheme. Reported barriers included digital infrastructure gaps, policy misalignment, lack of data protection policies and workforce limitations. Although the SPICE app, central to the Akoma Pa digital health program, enhanced patient tracking and care coordination, it still required ongoing support to ensure interoperability and scalability. Evidence-based practices and personalized care improved patient management and outcomes. CONCLUSION: Integrated mHealth programs such as Akoma Pa hold promise for strengthening chronic disease management in low-resource settings. Addressing infrastructural and long-term funding barriers is critical to sustaining and scaling these interventions. Findings offer insights to inform future digital health policy and program design in sub-Saharan Africa.
Dit artikel is een samenvatting van een publicatie in BMC health services research. Voor het volledige artikel, alle details en referenties verwijzen wij u naar de oorspronkelijke bron.
Lees het volledige artikelDOI: 10.1186/s12913-026-14175-0
