Niergezondheid en bloeddruk op schoolleeftijd na zeer vroeggeboorte
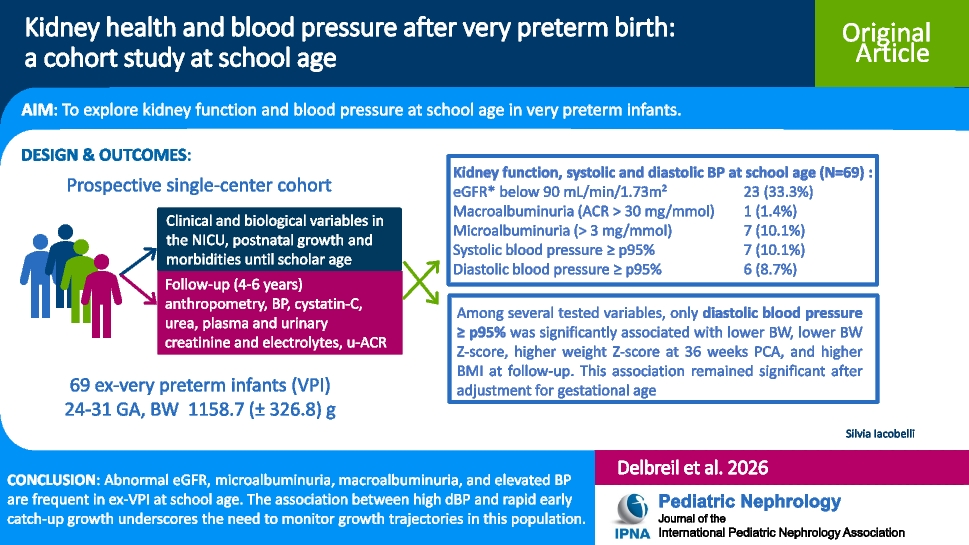
Een cohortonderzoek bij schoolgaande kinderen die zeer prematuur werden geboren (onder 32 weken) toonde subtiele afwijkingen in nierfunctie en bloeddruk. Deze vroege veranderingen kunnen voorafgaan aan klinisch manifeste nierziekte op latere leeftijd.
Perinatale en postnatale factoren, waaronder neonatale voeding en groei, bleken hiermee geassocieerd.
Abstract (original)
BACKGROUND: Very preterm infants (VPI, < 32 weeks of gestation) are at increased risk of chronic kidney disease and hypertension in later life, and slight abnormalities of kidney function may precede clinically apparent disease. We explored kidney function and blood pressure (BP) at school age in VPI, and their association with perinatal and postnatal factors, including neonatal nutrition and growth. METHODS: All VPI included at birth in a historical cohort evaluating kidney function during the first month of life were eligible at follow-up (4-6 years). Standardized assessments included anthropometry, BP, cystatin-C, urea, plasma and urinary creatinine and electrolytes, and urinary albumin-to-creatinine ratio. Abnormal biological findings were defined as one among: estimated glomerular filtration rate (eGFR) < 90 mL/min/1.73 m2, macroalbuminuria, or microalbuminuria. RESULTS: We included 69 children (mean age 5.1 ± 0.3 years). Thirty-one (44.9%) had at least one abnormal finding: eGFR < 90 mL/min/1.73 m2 (33.8%), macroalbuminuria (1.4%), microalbuminuria (10.1%). High systolic and diastolic pressure (dBP) occurred in 10.1% and 8.7% of children, respectively. No variables were associated with abnormal eGFR, microalbuminuria, or macroalbuminuria. High dBP was significantly associated with lower birth weight (BW), lower (BW) Z-score, higher weight Z-score at 36 weeks post-conception, and higher BMI at follow-up. This association remained significant after adjustment for gestational age. CONCLUSIONS: Abnormal eGFR, microalbuminuria, macroalbuminuria, as well as elevated BP are frequent in ex-VPI at school age. The association between high dBP and rapid early catch-up growth underscores the need to monitor growth trajectories as part of early kidney and cardiovascular risk assessment in this population.
Dit artikel is een samenvatting van een publicatie in Pediatric nephrology (Berlin, Germany). Voor het volledige artikel, alle details en referenties verwijzen wij u naar de oorspronkelijke bron.
Lees het volledige artikelDOI: 10.1007/s00467-026-07190-0